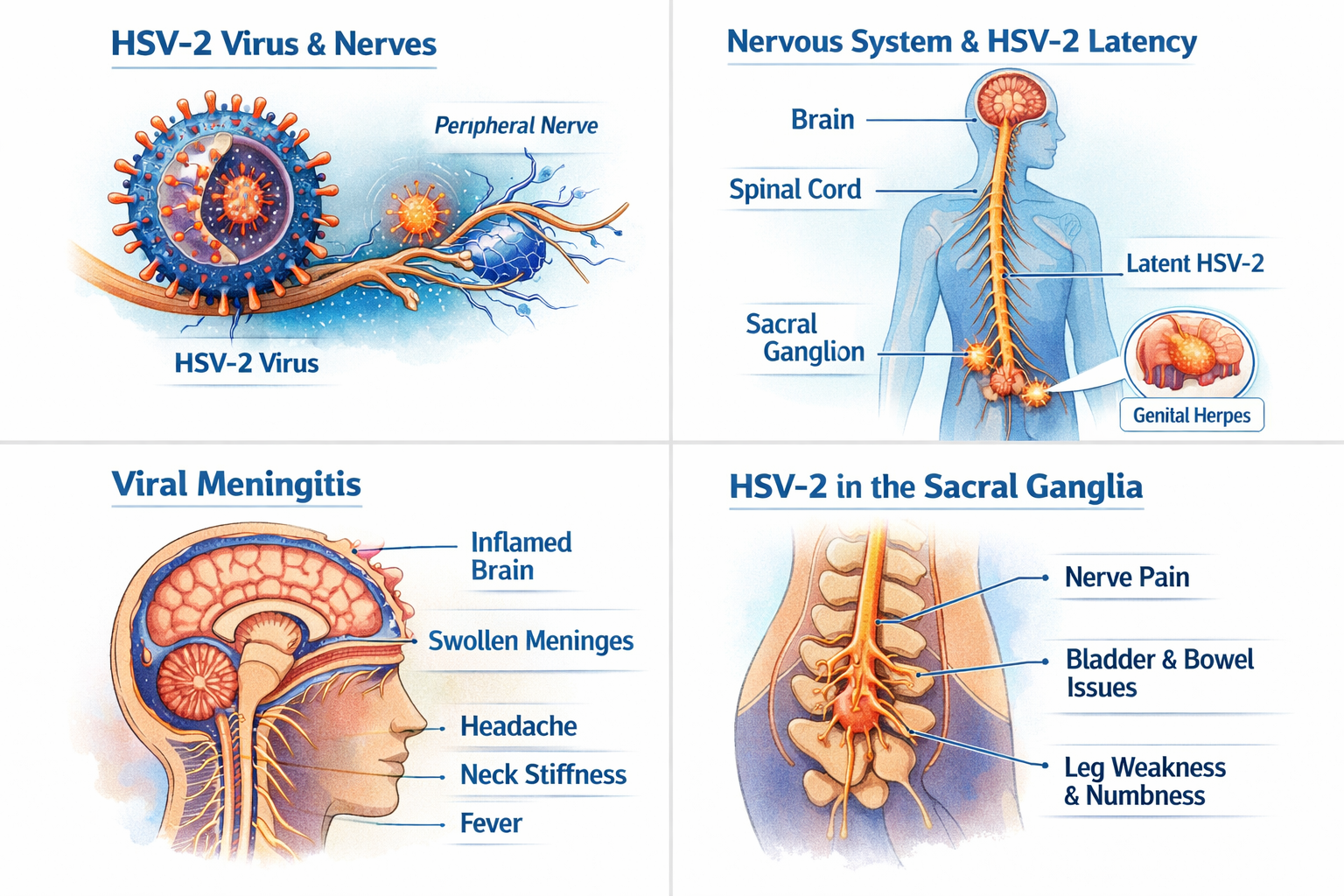
HSV-2 and Your Nerves
Neurological Complications of Herpes Simplex Virus Type 2 (HSV-2)
Introduction
Herpes Simplex Virus Type 2 is most commonly recognized for causing genital herpes, a lifelong viral infection characterized by recurrent outbreaks. However, beyond its dermatological presentation, HSV-2 has the capacity to affect the nervous system in ways that are often under-discussed yet clinically significant.
This article explores the neurological complications associated with HSV-2, shedding light on how a virus typically linked to the skin can impact deeper, more complex systems within the body.
How HSV-2 Interacts with the Nervous System
After initial infection, HSV-2 travels along peripheral nerves and establishes latency in the sacral nerve ganglia. During reactivation, the virus can travel back along these nerve pathways, sometimes leading not only to skin lesions but also to neurological symptoms.
This neurotropic behavior—meaning the virus has an affinity for nerve tissue—is central to understanding its complications.
Key Neurological Complications
1. Viral Meningitis
One of the most recognized neurological effects of HSV-2 is Viral Meningitis, particularly a recurrent form known as Mollaret’s meningitis.
Symptoms may include:
Severe headache
Neck stiffness
Sensitivity to light
Fever
Nausea and vomiting
Unlike bacterial meningitis, HSV-2 meningitis is often self-limiting but can recur, creating cycles of distress for affected individuals.
2. Sacral Radiculitis (Elsberg Syndrome)
Elsberg Syndrome is a lesser-known but important complication involving inflammation of the lower spinal nerve roots.
Clinical features:
Lower back or sacral pain
Urinary retention or difficulty
Constipation
Leg weakness or sensory changes
This condition directly reflects HSV-2’s tendency to reside in sacral ganglia.
3. Peripheral Neuropathy
HSV-2 may contribute to nerve irritation or damage, leading to symptoms consistent with Peripheral Neuropathy.
Common experiences:
Tingling or burning sensations
Shooting nerve pain
Hypersensitivity in affected areas
These symptoms may occur during outbreaks or persist in some individuals between episodes.
4. Encephalitis (Rare)
While more commonly associated with HSV-1, Encephalitis caused by HSV-2 can occur, particularly in immunocompromised individuals.
Potential signs:
Altered mental status
Confusion or memory issues
Seizures
Behavioral changes
This is a medical emergency requiring immediate antiviral treatment.
Psychological and Neurocognitive Impact
Beyond direct neurological damage, HSV-2 can contribute to psychological stress, which may indirectly affect cognitive function. Chronic anxiety, stigma, and recurring symptoms can influence sleep, focus, and emotional regulation.
Diagnosis and Management
Neurological complications of HSV-2 are typically diagnosed through:
Clinical evaluation
Cerebrospinal fluid (CSF) analysis
PCR testing for viral DNA
Treatment approaches include:
Antiviral medications such as Acyclovir, Valacyclovir, or Famciclovir
Pain management strategies
Supportive neurological care
Early intervention improves outcomes, particularly in severe cases.
Final Thoughts
HSV-2 is more than a skin-level condition. Its ability to interact with the nervous system highlights the importance of awareness, early recognition, and appropriate care. While many neurological complications are rare or manageable, understanding their presence empowers individuals and clinicians to respond effectively.
In the broader conversation of health, HSV-2 reminds us that what appears external often has deeper internal dimensions—requiring both medical insight and compassionate understanding.